The 20-Minute Pilonidal Cyst Procedure That Gets Patients Back to Normal in Days, Not Weeks
Dual board-certified surgeon now offers a minimally invasive technique studied on over 2,300 patients that most patients have never heard of. If you're living with a painful, recurring pilonidal cyst, read this now.
"Why Won't This Thing Go Away?"
If you've ever sat in a chair and felt that sharp, throbbing pain near your tailbone, the one that makes you shift your weight every few minutes, dread long car rides, and silently pray nobody asks why you're standing at your desk, you already know what a pilonidal cyst feels like.
And if you've had one drained, felt the relief, only to have it come roaring back weeks or months later... you know the frustration that comes with it.
You're not alone. Pilonidal disease affects roughly 26 out of every 100,000 people, and it overwhelmingly strikes young, active adults between 15 and 35: people who sit for school, work, or sport. People who can't afford to be out of commission for weeks.
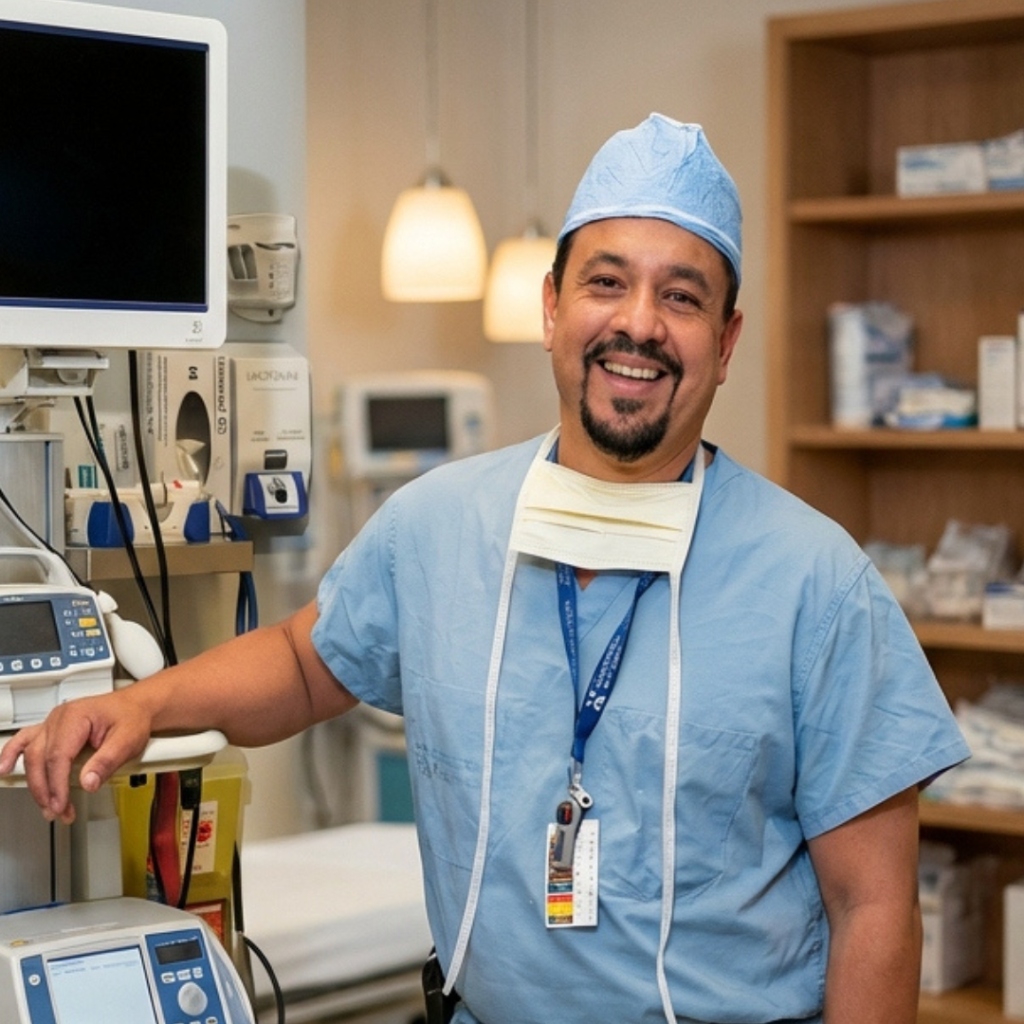
My name is Dr. Hector Roldan. I'm a dual board-certified general surgeon and Fellow of both the Royal College of Physicians and Surgeons of Canada (FRCSC) and the American College of Surgeons (FACS), and I serve as a General Surgeon & Cosmetic Medicine Specialist at Muskoka Algonquin Healthcare.
Over 25 years of surgical practice and more than 5,000 procedures, I've treated over 175 patients with pilonidal disease. And what I kept seeing disturbed me.
The Pattern I Couldn't Ignore
I started noticing something troubling. The same young patients (university students, tradespeople, office workers) kept returning to my clinic after being treated elsewhere for pilonidal cysts.
They'd had one drainage. Then another. Then another. Some had already undergone full excision surgery at other facilities and were back with a recurrence, now dealing with a large scar and the same problem.
These weren't patients who had done anything wrong. They'd followed their doctors' advice. They'd kept the area clean. They'd taken their antibiotics. The treatments themselves were failing them.
So I did what I always do when I see a pattern that doesn't make sense: I started researching. And what I found changed how I treat this condition entirely.
What's Actually Happening Under Your Skin (And Why Nobody Explains This)
A pilonidal cyst forms in the natal cleft (the crease between the buttocks) when loose hairs are driven into the skin through tiny pits. Your body treats these as foreign invaders and mounts an inflammatory response, creating a pocket of infected tissue beneath the skin.
Over time, this pocket forms tunnels called sinus tracts that burrow beneath the surface. These tracts accumulate hair, debris, and bacteria, creating a chronic inflammatory environment your body cannot resolve on its own.
Enters Skin
Reaction
Form
Inflammation
Why Everything You've Tried Hasn't Worked
Incision & Drainage (I&D)
- Relieves acute infection, nothing more
- Does not remove the sinus tracts that caused the problem
- Recurrence rate (16-mo follow-up): approximately 40%
Traditional Wide Excision Surgery
- Cuts out the entire cyst and a large margin of surrounding tissue
- Leaves a significant open wound: 6-12 weeks to heal
- Requires daily wound packing, often painful
- Recurrence rate (16-mo follow-up): 10-30%
- Extended time away from work, school, and life
Antibiotics & "Wait and See"
- Cannot dissolve sinus tracts: the lining remains intact
- Delays definitive treatment while disease worsens
- Risks development of more complex sinus networks
A Surgical Option Many Patients Haven't Been Offered: The Gips Procedure
In 2008, Dr. Moshe Gips published a landmark paper in Diseases of the Colon & Rectum describing a minimally invasive technique developed while treating 1,358 patients over a 10-year period at a dedicated surgical clinic. Rather than cutting out large sections of tissue, it does something much more precise:
It targets and removes only the diseased tissue (the pits, tracts, and debris) while leaving healthy tissue intact.
The Clinical Evidence
(Di Castro et al., Int J Surg, 2016)
(Di Castro et al., Int J Surg, 2016)
(Di Castro et al., Int J Surg, 2016)
In Dr. Gips' original series of 1,358 patients, complete healing occurred within 3.4 weeks, compared to 6-12 weeks for traditional excision (Gips et al., Diseases of the Colon & Rectum, 2008). A study on adolescent patients found the mean return to daily activities and school was just 2 days, with a mean operative time of 14 minutes (Turkyilmaz et al., Cutis, 2020).
| Factor | Traditional Excision | I&D | Gips Procedure |
|---|---|---|---|
| Anesthesia | General/regional | Local | Local |
| Procedure time | 45-90 min | 15-20 min | ~20 min |
| Wound size | Large open wound | Small incision | Tiny trephine holes |
| Daily packing | Yes, weeks | Often yes | No |
| Return to activity | 4-8 weeks | 1-2 weeks | 1-3 days |
| Recurrence | 10-30% | ~40% | 5.8% |
Note: Recurrence data for the Gips procedure reflects median 16-month follow-up (Di Castro et al., 2016). A 2023 systematic review notes that longer-term recurrence rates may be higher, and individual outcomes depend on the extent of disease and post-operative hair management compliance.
Your Recovery Timeline
Imagine This
Imagine sitting through an entire eight-hour workday without shifting in your chair. Driving to the cottage on a Friday evening without dreading every bump. Sitting in a lecture hall, at a hockey game, on a long flight, without that constant, nagging awareness that something is wrong.
Imagine not cancelling plans because of a flare-up. Not Googling "pilonidal cyst won't go away" at 2 AM. Not explaining to your boss why you need another day off for another drainage.
Imagine your teenager going back to school on Monday after a Friday procedure, instead of missing six weeks of classes.
This is what definitive treatment looks like. Not another round of antibiotics. Not another temporary drain. A real solution that addresses the disease at its source.
This is about getting your life back, not just treating a symptom.
About Dr. Roldan's Practice
Why Dr. Roldan Is Uniquely Qualified
- Dual board certification, FRCSC and FACS, the highest standards in both Canada and the US
- 25+ years, 5,000+ procedures
- Honest consultations: complete evaluation, all options discussed, no pressure
What the Cycle of Failed Treatment Actually Costs You
- Multiple ER visits (parking, time, travel, indirect costs) each time
- Lost wages: 2-3 days per flare-up, multiple times per year
- Prescriptions and wound supplies, repeatedly
- Traditional excision: 4-8 weeks away from work or school
- The emotional cost: anxiety, embarrassment, diminished quality of life
You Have Three Options
How to Get Started
- Examine your condition and assess the extent of disease
- Explain all treatment options clearly and honestly
- Recommend the best approach for your long-term outcome
- Answer every question, no rush, no pressure
To your health and recovery,
Fellow, Royal College of Physicians and Surgeons of Canada
Fellow, American College of Surgeons
25+ Years of Surgical Practice
Frequently Asked Questions
P.S. If you've had a pilonidal cyst drained once or more and it keeps coming back, there's a reason: drainage doesn't remove the sinus tracts. The Gips procedure specifically targets and removes those tracts. Don't wait for the next flare-up. Call 705.789.1874.
P.P.S. If you're a parent and your teenager is dealing with a pilonidal cyst, this procedure has been specifically studied in adolescent patients with excellent results and minimal school disruption. Schedule a consultation for your child here.
References
- Di Castro A, Guerra F, Levi Sandri GB, Ettorre GM. Minimally invasive surgery for the treatment of pilonidal disease. The Gips procedure on 2347 patients. Int J Surg. 2016;36(Pt A):201-205.
- Gips M, Melki Y, Salem L, Weil R, Sulkes J. Minimal surgery for pilonidal disease using trephines: description of a new technique and long-term outcomes in 1,358 patients. Dis Colon Rectum. 2008;51:1656-1662.
- Turkyilmaz Z, Karabulut R, Oral H, Muradi T, Altin M, Sonmez K. The Gips procedure for pilonidal disease: a retrospective review of adolescent patients. Cutis. 2020;106:261-264.
- Johnson EK, Vogel JD, Cowan ML, et al. The American Society of Colon and Rectal Surgeons' clinical practice guidelines for the management of pilonidal disease. Dis Colon Rectum. 2019;62(2):146-157.
- Stable I, Coscia M, Nascimbeni R, et al. Minimally invasive surgery for pilonidal disease: Outcomes of the Gips technique. A systematic review and meta-analysis. Surgery. 2023;174(4):882-889.
Medical Disclaimer
This is a paid advertisement for the surgical practice of Dr. Hector Roldan, MD, FRCSC, FACS. This information is for educational purposes and does not constitute medical advice. Individual results vary. Not all patients are candidates for the Gips procedure. A consultation with Dr. Roldan is required to determine the best treatment. All surgery carries risks including infection, bleeding, and recurrence. Clinical data cited reflects published, peer-reviewed research (Di Castro et al., Int J Surg, 2016; Gips et al., Dis Colon Rectum, 2008; Turkyilmaz et al., Cutis, 2019) and may not represent every individual outcome. Individual results depend on the nature and extent of disease, patient health, and adherence to post-operative care.
Results Disclaimer
Recovery times are based on published studies and represent typical results. Individual healing varies based on disease extent, health, and adherence to post-operative care.
Articles © 2026 Dr. Hector Roldan MD. All right